FUNGAL INFECTIONS
Fungal diseases are caused by various types of fungi and can affect humans, animals, plants, and even ecosystems. Examples include athlete’s foot, ringworm, and candidiasis in humans. In agriculture, fungi can cause crop diseases, impacting food production. Effective management involves antifungal medications for human health and fungicides in agriculture. Understanding fungal biology is crucial for developing targeted treatments and preventive measures.
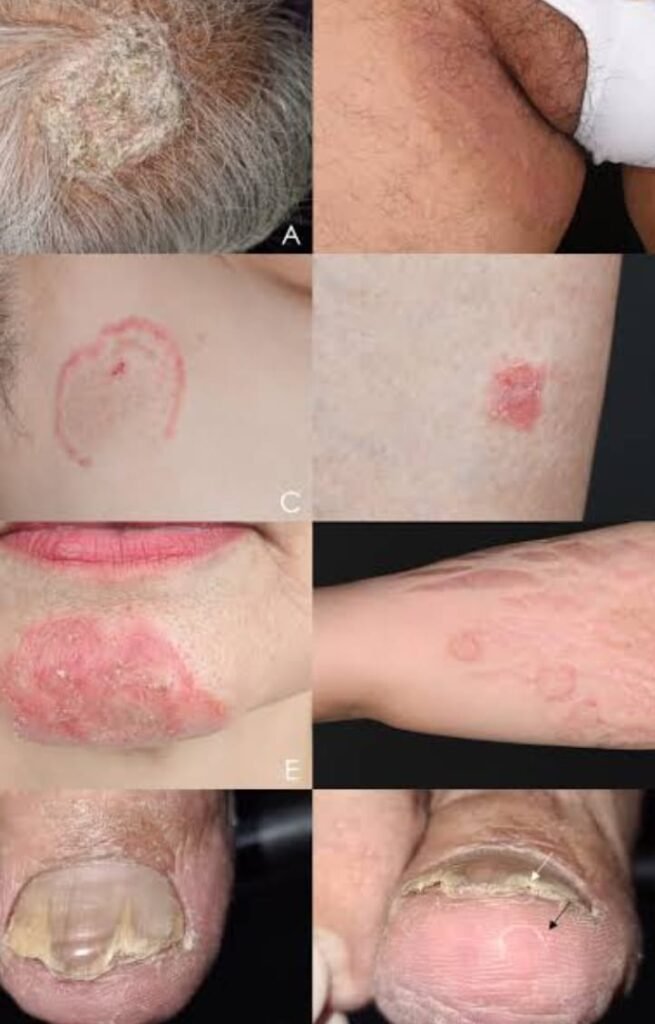
TYPES OF FUNGAL INFECTION
There are thousands of fungal species, and they can cause a diverse range of diseases in humans, animals, plants, and other organisms. It’s challenging to provide an exact number of types of fungal diseases due to the vast diversity of fungi and their ability to affect different hosts. Common examples in humans include dermatophyte infections, candidiasis, and aspergillosis. In agriculture, fungi can cause various plant diseases. Each type of fungus may have multiple strains or varieties, contributing to the complexity of fungal diseases.
Certainly, here are some common fungal infections in humans:
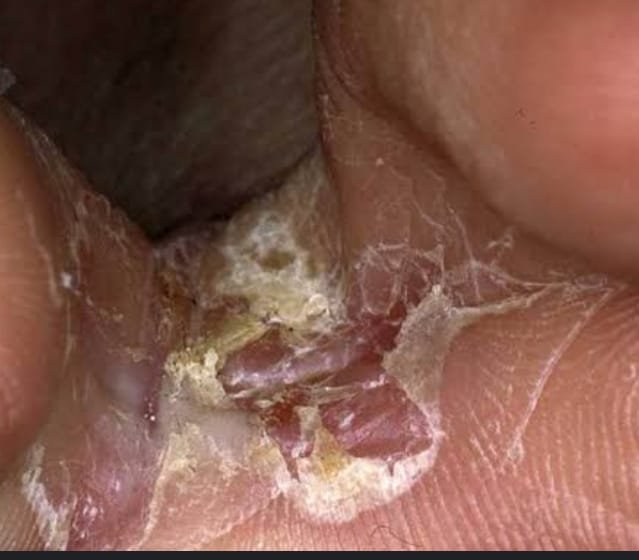
- Athlete’s Foot (Tinea Pedis): Affects the feet, causing itching and peeling.
- Ringworm (Tinea Corporis): Circular, red skin rashes on various body parts.
- Jock Itch (Tinea Cruris): Occurs in the groin area, leading to itching and discomfort.
- Candidiasis: Includes yeast infections like oral thrush and genital yeast infections.
- Aspergillosis: Caused by the Aspergillus fungus, often affecting the lungs.
- Cryptococcosis: Affects the lungs and central nervous system, often in immunocompromised individuals.
- Histoplasmosis: Inhaled from soil containing bird or bat droppings, impacting the lungs.
- Coccidioidomycosis (Valley Fever): Respiratory infection caused by inhaling spores in certain regions.
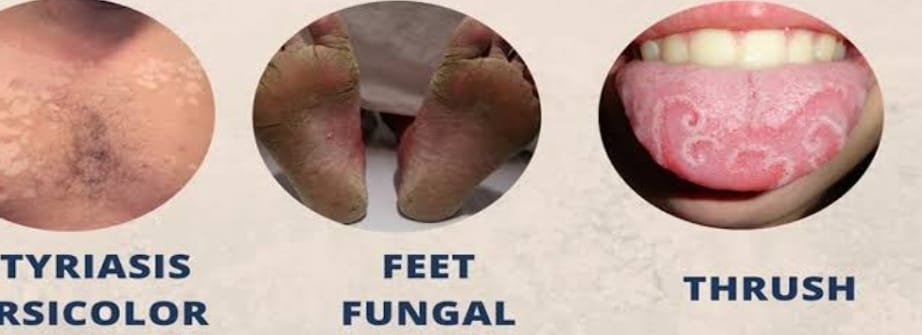
It’s important to note that specific types of fungi can cause these infections, and severity can vary. Always consult a healthcare professional for accurate diagnosis and treatment.
HOW TO PREVENT FROM THIS
To prevent fungal diseases, consider the following measures:
- Personal Hygiene:
- Keep skin dry and clean.
- Regularly wash hands, especially before handling food.
- Foot Care:
- Dry feet thoroughly, especially between toes.
- Wear breathable shoes and moisture-wicking socks.
- Avoid Sharing Personal Items:
- Do not share towels, combs, or other personal items.
- Manage Moisture:
- Keep living spaces well-ventilated.
- Use antifungal powders in areas prone to moisture.
- Diet and Immune Health:
- Maintain a balanced diet to support immune function.
- Manage underlying health conditions that can weaken the immune system.
- Protective Clothing:
- Wear appropriate clothing in environments where fungi may be present (gardens, construction sites).
- Avoiding Contaminated Environments:
- Be cautious in environments with a high risk of fungal exposure, such as construction sites or certain agricultural settings.
- Properly Treat Infections:
- Promptly treat any existing fungal infections under the guidance of a healthcare professional.
- Routine Checkups:
- Regularly check for signs of fungal infections, especially if you have risk factors.
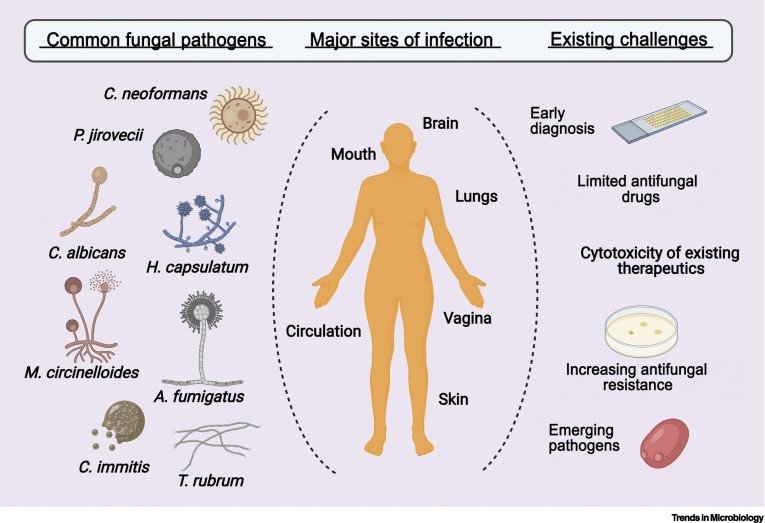
Remember, prevention strategies may vary depending on the specific type of fungal infection and the host organism. If you suspect an infection, consult a healthcare provider for proper diagnosis and treatment.
DIAGNOSIS AND TREATMENT
If you suspect a fungal infection, it’s essential to consult with a healthcare professional for an accurate diagnosis and appropriate treatment. However, here are some general steps you can take:
- See a Doctor: Schedule an appointment with a healthcare provider, such as a dermatologist or general practitioner, to get a proper diagnosis.
- Provide Details: Be prepared to provide information about your symptoms, when they started, any potential exposure to fungi, and any treatments you may have tried.
- Follow Medical Advice: Once diagnosed, follow the prescribed treatment plan. This may include antifungal medications, creams, or ointments.
- Maintain Good Hygiene: Keep the affected area clean and dry. Follow any specific hygiene recommendations provided by your healthcare provider.
- Avoid Self-Treatment: Refrain from self-diagnosis and self-treatment with over-the-counter medications without professional guidance, as it may worsen the condition.
- Complete the Treatment: Finish the entire course of prescribed medication, even if symptoms improve before completion. This helps prevent the recurrence of the infection.
- Prevent Spread: Take precautions to avoid spreading the infection to others. This may include avoiding sharing personal items and practicing good hand hygiene.
- Address Underlying Factors: If the fungal infection is recurrent or persistent, your healthcare provider may explore underlying health conditions or contributing factors that need addressing.
Remember, individual cases may vary, and professional medical advice is crucial for effective management of fungal infections.
PRECAUTIONS
To prevent fungal infections and protect your overall health, consider these precautions:
- Maintain Personal Hygiene:
- Wash your hands regularly, especially before handling food.
- Keep skin clean and dry, paying attention to areas prone to moisture.
- Foot Care:
- Keep feet dry, especially between toes.
- Choose breathable footwear and moisture-wicking socks.
- Avoid Sharing Personal Items:
- Do not share towels, combs, or other personal items.
- Manage Moisture:
- Ensure living spaces are well-ventilated.
- Use antifungal powders in areas prone to moisture, such as shoes.
- Healthy Diet:
- Maintain a balanced diet rich in nutrients to support your immune system.
- Protective Clothing:
- Wear appropriate clothing in environments where fungal exposure is likely.
- Regular Checkups:
- Monitor for any signs of fungal infections and seek prompt medical attention if needed.
- Limit Exposure in Risky Environments:
- Be cautious in environments where fungi may thrive, such as construction sites or areas with decaying organic matter.
- Stay Informed:
- Educate yourself about common fungal infections and their preventive measures.
- Manage Underlying Conditions:
- If you have underlying health conditions that may compromise your immune system, work with healthcare professionals to manage them effectively.
Remember, these precautions are general guidelines. If you suspect a fungal infection or have specific concerns, consult with a healthcare provider for personalized advice based on your health status and lifestyle.

MEDICATIONS
The treatment of fungal diseases typically involves antifungal medications. The specific medication and form of treatment depend on the type of fungal infection, its severity, and the affected area. Here are some common approaches:
- Topical Antifungals:
- Creams, ointments, or powders applied directly to the skin for superficial infections like athlete’s foot or ringworm.
- Oral Antifungals:
- Prescribed for more severe or systemic infections, such as oral thrush or fungal nail infections.
- Antifungal Shampoos:
- Used for fungal infections of the scalp or hair, like ringworm of the scalp.
- Intravenous (IV) Antifungals:
- Administered through a vein for severe systemic infections, especially in immunocompromised individuals.
- Antifungal Nail Lacquer:
- Applied directly to the affected nails for fungal nail infections.
- Combination Therapies:
- In some cases, a healthcare provider may recommend a combination of topical and oral antifungal treatments.
It’s crucial to follow the prescribed treatment plan, complete the entire course of medication, and attend follow-up appointments as advised by your healthcare provider. Even if symptoms improve before the treatment is finished, completing the course helps prevent recurrence and ensures the complete elimination of the fungus.
In cases of recurrent or persistent infections, additional tests and investigations may be needed to identify underlying factors contributing to the susceptibility to fungal infections. Always consult a healthcare professional for personalized advice and treatment.

I am a content writer I have experience been writing news and blog articles for 5 years.