HEART DISEASE
Heart disease, or cardiovascular disease, encompasses various conditions affecting the heart and blood vessels. Common types include coronary artery disease, heart failure, arrhythmias, and valvular heart diseases. Risk factors include high blood pressure, high cholesterol, smoking, obesity, and diabetes. Symptoms vary but may include chest pain, shortness of breath, fatigue, and irregular heartbeat. Diagnosis often involves medical history, physical exams, blood tests, imaging, and cardiac catheterization. Treatment may include lifestyle changes, medications, and procedures like angioplasty or bypass surgery. Regular check-ups and a healthy lifestyle can help prevent heart disease. Always consult with healthcare professionals for personalized advice.

HEART ATTACK
A heart attack, or myocardial infarction, occurs when blood flow to a part of the heart muscle is blocked, usually by a blood clot. This blockage can damage or destroy the affected part of the heart muscle. The process typically involves:
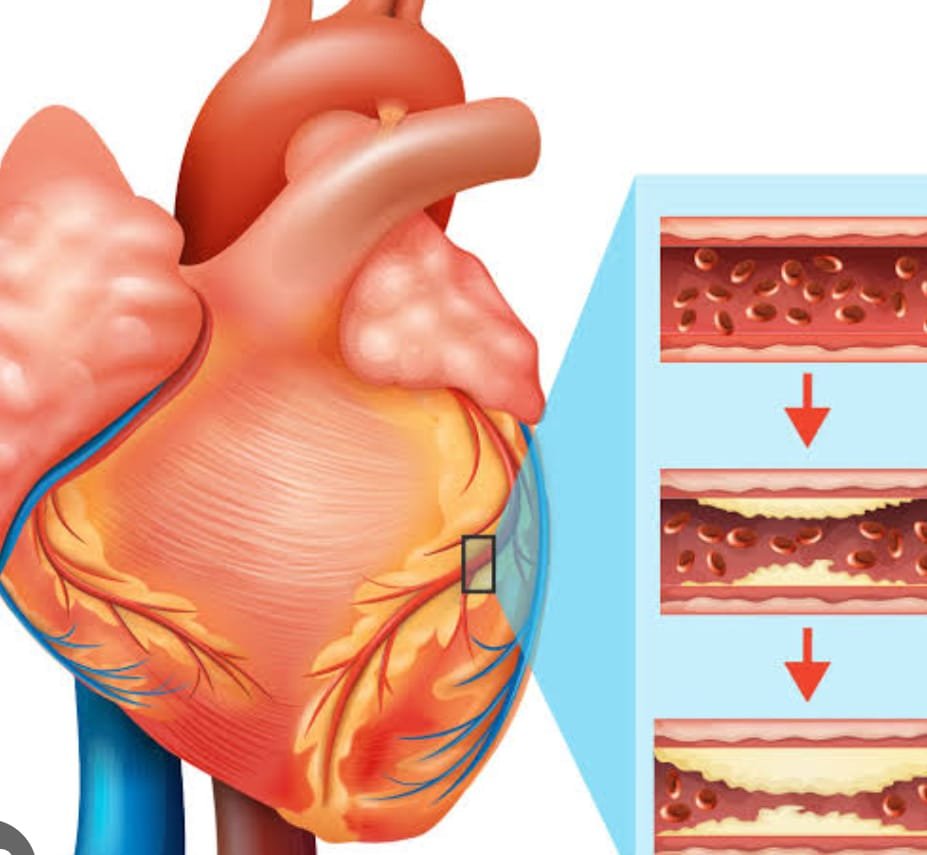
- Coronary Artery Disease (CAD): Atherosclerosis, the buildup of fatty deposits (plaque) in coronary arteries, is a common cause. Over time, this can narrow or block the arteries.
- Plaque Rupture: The plaque can rupture, causing a blood clot (thrombus) to form at the site. This clot can obstruct blood flow through the coronary artery.
- Ischemia: The blocked artery leads to reduced blood supply (ischemia) to a part of the heart muscle. Without prompt intervention, the affected tissue can die.
- Symptoms: Common symptoms include chest pain or discomfort, shortness of breath, nausea, and lightheadedness.
- Medical Emergency: Prompt medical attention is crucial. Emergency treatments may include medications to dissolve clots, angioplasty to open blocked arteries, or bypass surgery.
Reducing risk factors such as smoking, maintaining a healthy diet, exercising, and managing conditions like hypertension and diabetes can help prevent heart attacks. Regular check-ups with healthcare professionals aid in early detection and prevention.
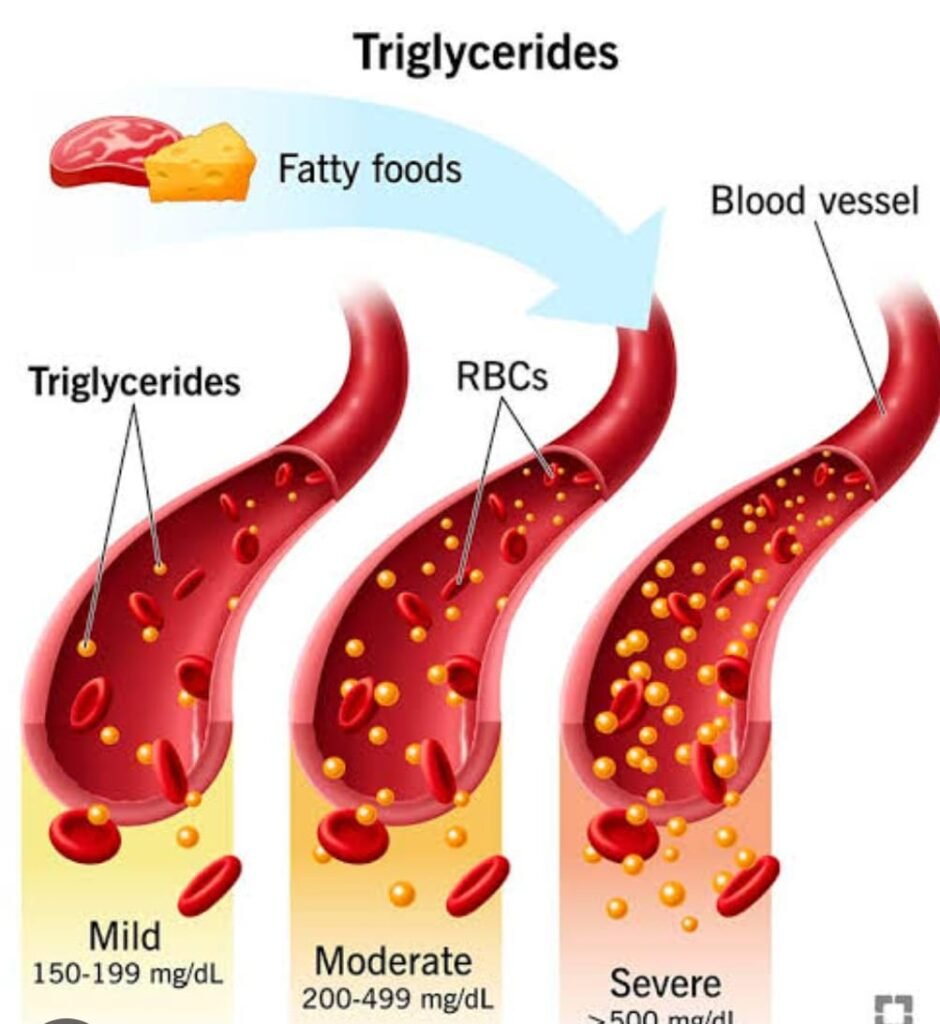
TRIGLYCERIDES
Triglycerides are a type of fat (lipid) found in your blood. They are the most common type of fat in the body and are essential for energy storage. Triglycerides come from the food you eat, especially from fats and carbohydrates.
Here’s a brief overview:
- Source: Triglycerides come from the fats and oils in the food we eat. Excess calories, especially from carbohydrates, can be converted into triglycerides and stored in fat cells.
- Transport: Triglycerides circulate in the bloodstream and are used by the body for energy between meals. They are also stored in fat cells to be released when energy is needed.
- Levels: Elevated triglyceride levels can be associated with an increased risk of heart disease. High levels may be caused by factors such as obesity, poorly controlled diabetes, a sedentary lifestyle, or a diet high in sugars and refined carbohydrates.
- Testing: A blood test, often done after fasting, can measure triglyceride levels. The test is usually part of a lipid panel that also measures cholesterol levels.
- Healthy Levels: Normal triglyceride levels are generally considered to be less than 150 milligrams per deciliter (mg/dL). However, optimal levels for heart health may be lower.
Managing triglyceride levels involves adopting a healthy lifestyle, including a balanced diet, regular physical activity, maintaining a healthy weight, and avoiding excessive alcohol intake. If triglyceride levels are significantly elevated, healthcare professionals may recommend medications as well.
RISK FACTORS
Reducing risk factors such as smoking, maintaining a healthy diet, exercising, and managing conditions like hypertension and diabetes can help prevent heart attacks. Regular check-ups with healthcare professionals aid in early detection and prevention.
Several risk factors contribute to the development of heart disease. These can be categorized into modifiable and non-modifiable factors. Understanding and addressing these factors is crucial for prevention. Here are some key risk factors:
Non-Modifiable Risk Factors:
- Age: The risk of heart disease increases with age.
- Gender: Men, especially those over 45, have a higher risk. Women’s risk increases after menopause.
- Genetics/Family History: If close family members had heart disease, the risk may be higher.
Modifiable Risk Factors:
- High Blood Pressure: Hypertension strains the heart and arteries, increasing the risk of heart disease.
- High Cholesterol: Elevated levels of LDL (“bad”) cholesterol and low levels of HDL (“good”) cholesterol can contribute to plaque buildup in arteries.
- Smoking: Tobacco smoke contains chemicals that can damage blood vessels and heart tissue.
- Obesity: Being overweight or obese puts additional strain on the heart and is often linked to other risk factors.
- Diabetes: People with diabetes are at an increased risk of heart disease.
- Physical Inactivity: Lack of regular exercise is a significant risk factor.
- Unhealthy Diet: Diets high in saturated fats, trans fats, sodium, and low in fruits, vegetables, and whole grains contribute to heart disease.
- Excessive Alcohol Consumption: Heavy drinking can raise blood pressure and contribute to heart failure.
- Stress: Chronic stress may contribute to heart disease, although the link is complex.
- Sleep Apnea: Untreated sleep apnea can contribute to high blood pressure and other cardiovascular issues.
Addressing modifiable risk factors through lifestyle changes, medications, and regular medical check-ups is crucial for preventing heart disease. It’s essential to consult with healthcare professionals for personalized advice and risk assessment.
CHOLESTEROL
Cholesterol is a fatty substance that is essential for building cells and producing certain hormones. It is found in the cells of your body and in the food you eat. Cholesterol travels through the bloodstream in small packages called lipoproteins, which can be high-density lipoproteins (HDL), low-density lipoproteins (LDL), and very-low-density lipoproteins (VLDL).
Here’s a brief overview:
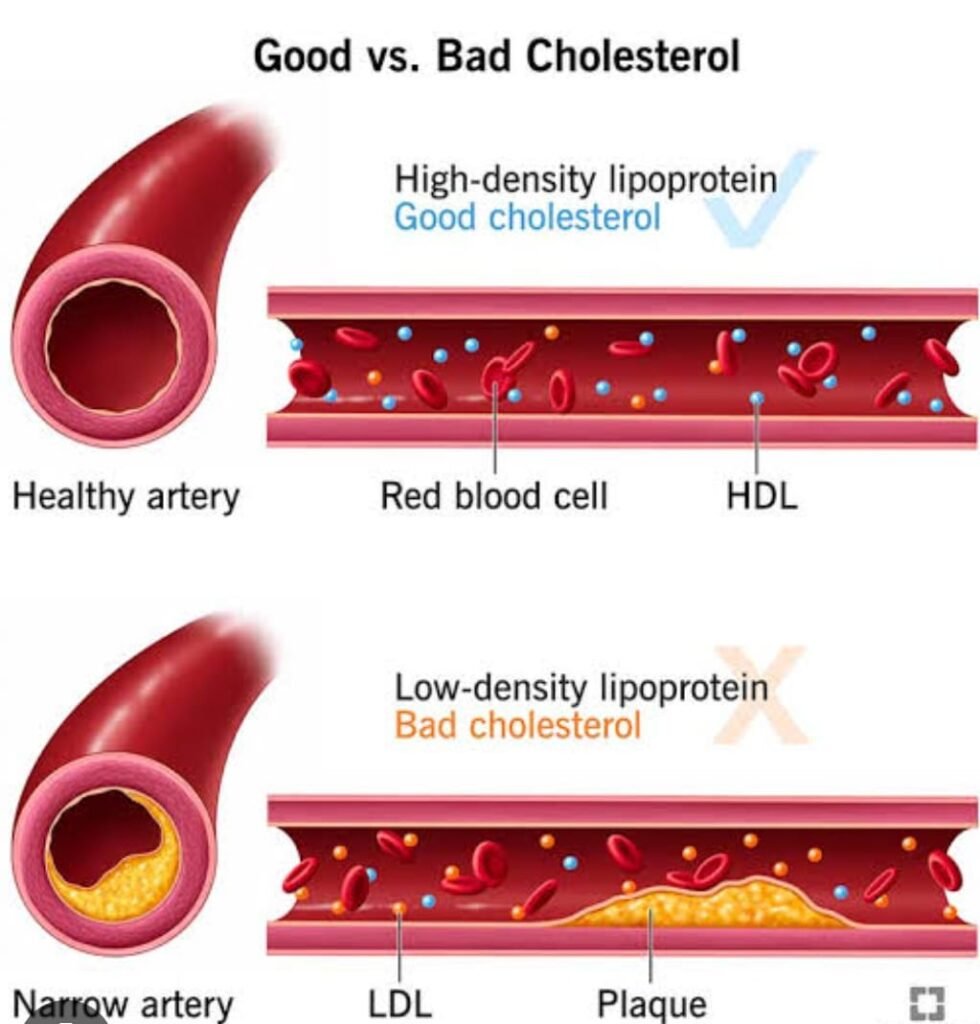
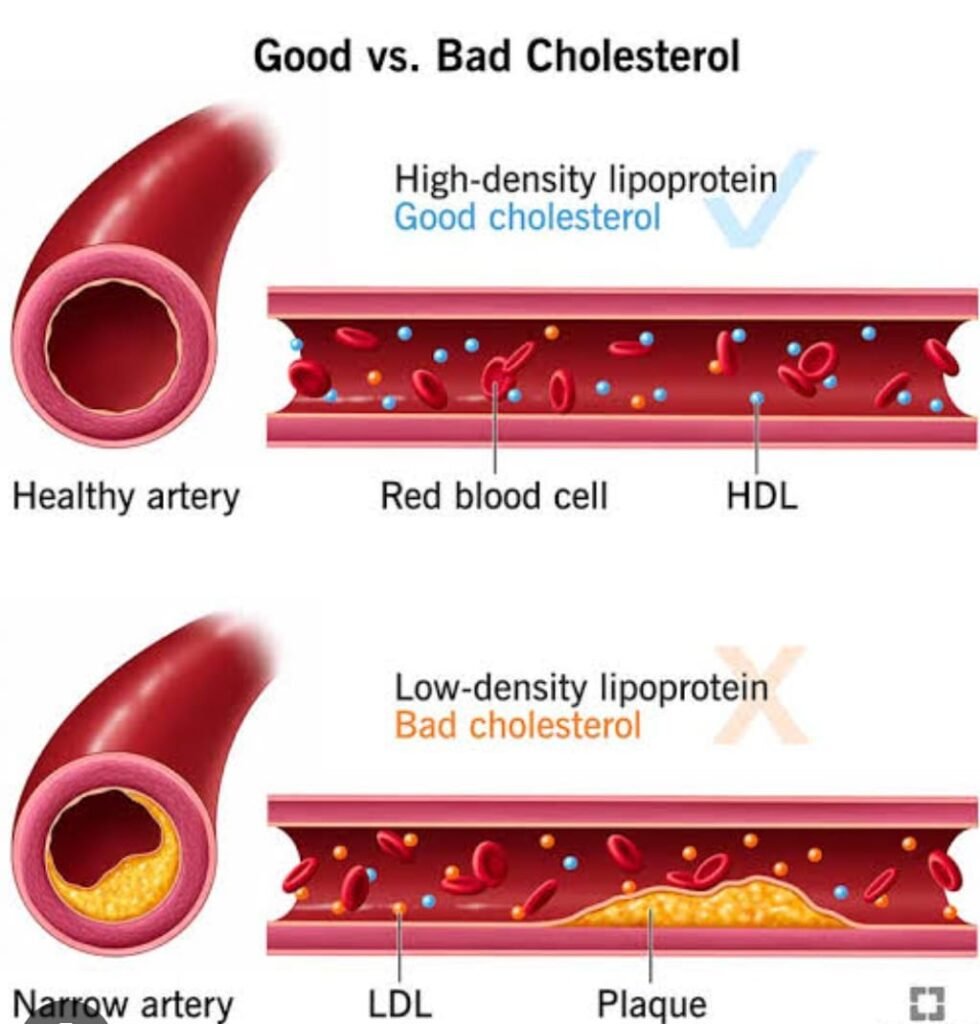
- HDL (High-Density Lipoprotein): Often referred to as “good” cholesterol, HDL helps remove excess cholesterol from your blood vessels and transport it to the liver for excretion.
- LDL (Low-Density Lipoprotein): Known as “bad” cholesterol, LDL carries cholesterol to the cells. If too much is delivered, it can build up in the walls of the arteries, leading to atherosclerosis.
- VLDL (Very-Low-Density Lipoprotein): Similar to LDL, VLDL carries triglycerides, a type of fat, in the blood. As VLDL triglycerides are broken down, they release LDL cholesterol.
- Cholesterol Testing: A blood test, commonly known as a lipid panel, measures total cholesterol, HDL, LDL, and triglycerides. This test is usually done after fasting.
- Healthy Levels: Optimal cholesterol levels contribute to heart health. Desirable total cholesterol is generally considered to be below 200 mg/dL, with higher levels of HDL and lower levels of LDL.
- Diet and Lifestyle: Eating a healthy diet, exercising regularly, maintaining a healthy weight, and avoiding smoking are crucial for managing cholesterol levels.
If cholesterol levels are outside the healthy range, healthcare professionals may recommend lifestyle changes, medications, or a combination of both to lower the risk of cardiovascular diseases. Regular monitoring and consultation with healthcare providers are essential for effective cholesterol management

PREVENTION FROM HEART DISEASE
Preventing heart disease involves adopting a heart-healthy lifestyle. Here are key measures:
- Healthy Diet: Consume a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats. Limit saturated and trans fats, cholesterol, sodium, and added sugars.
- Regular Exercise: Engage in regular physical activity, aiming for at least 150 minutes of moderate-intensity exercise per week. This helps maintain a healthy weight, lower blood pressure, and improve overall cardiovascular health.
- Maintain a Healthy Weight: Being overweight increases the risk of heart disease. Aim for a BMI within the healthy range and focus on sustainable weight management through diet and exercise.
- Quit Smoking: Smoking is a major risk factor for heart disease. Quitting reduces the risk and provides immediate and long-term health benefits.
- Limit Alcohol Intake: If you drink alcohol, do so in moderation. For most adults, this means up to one drink per day for women and up to two drinks per day for men.
- Manage Stress: Chronic stress can contribute to heart disease. Practice stress-reducing activities like meditation, deep breathing, yoga, or hobbies.
- Regular Health Check-ups: Schedule regular check-ups with healthcare professionals to monitor blood pressure, cholesterol levels, and other relevant indicators. Early detection and management of risk factors are crucial.
- Medication Compliance: If prescribed medications for conditions like hypertension or high bp

TREATMENT
The treatment for heart disease varies based on the specific condition but may include the following:
- Lifestyle Changes: Adopting a heart-healthy lifestyle is often the first line of defense. This includes a balanced diet, regular exercise, maintaining a healthy weight, quitting smoking, and moderating alcohol intake.
- Medications: Depending on the type of heart disease and its underlying causes, medications may be prescribed. These can include blood pressure medications, cholesterol-lowering drugs, antiplatelet agents, and medications to control heart rhythm.
- Interventional Procedures: In certain cases, procedures may be needed to treat or manage heart conditions. Examples include angioplasty to open blocked arteries, stent placement to keep arteries open, or bypass surgery to create new routes for blood flow.
- Device Implantation: Devices like pacemakers or implantable cardioverter-defibrillators (ICDs) may be recommended to regulate heart rhythm and prevent life-threatening arrhythmias.
- Cardiac Rehabilitation: This program involves supervised exercise, education, and counseling to help individuals recover from a heart-related event or procedure and improve overall cardiovascular health.
- Heart Transplant or Surgery: In severe cases, heart transplantation or surgical procedures like valve replacement or repair may be considered.
It’s crucial to note that treatment plans are individualized based on a person’s specific condition, medical history, and risk factors. Regular follow-ups with healthcare professionals are essential to monitor progress and adjust treatment as needed. Always consult with a healthcare provider for personalized advice and treatment recommendations.

I am a content writer I have experience been writing news and blog articles for 5 years.